The prediction of susceptibility to heritable breast, ovarian, and colon cancer raises important legal and ethical concerns. Health care professionals have a duty to disclose sufficient information to enable patients data. These duties may come into conflict if a positive finding in one patient implies that family members are also at risk. A legal distinction is made between a breach of confidentiality and the legitimate sharing of information in a patient’s interest or to prevent harm to a third party. Other issues concern the legal liability assumed by genetic counselors, whose disclosures may influence decisions about childbearing, for example, and the risk of socioeconomic discrimination faced by people with a known genetic susceptibility. Testing in children raises a different set of risks. Adults are able to choose for themselves about genetic testing after hearing the relative advantages and risks. Children, however, must rely on their parents to decide for them. Genetic testing requires additional considerations when done in the prenatal setting. In cases where there is no available medical therapy for a diagnosed genetic condition, the availability of limited options results in tough ethical choices for parents. To make these decisions, prospective parents need clear information regarding the meaning of test results. Ethical theories and principles provide a framework for resolving ethical dilemmas in maternal screening for genetic conditions during a pregnancy, carrier testing prior to or during a pregnancy, clinical genetic testing, and newborn metabolic screening. | 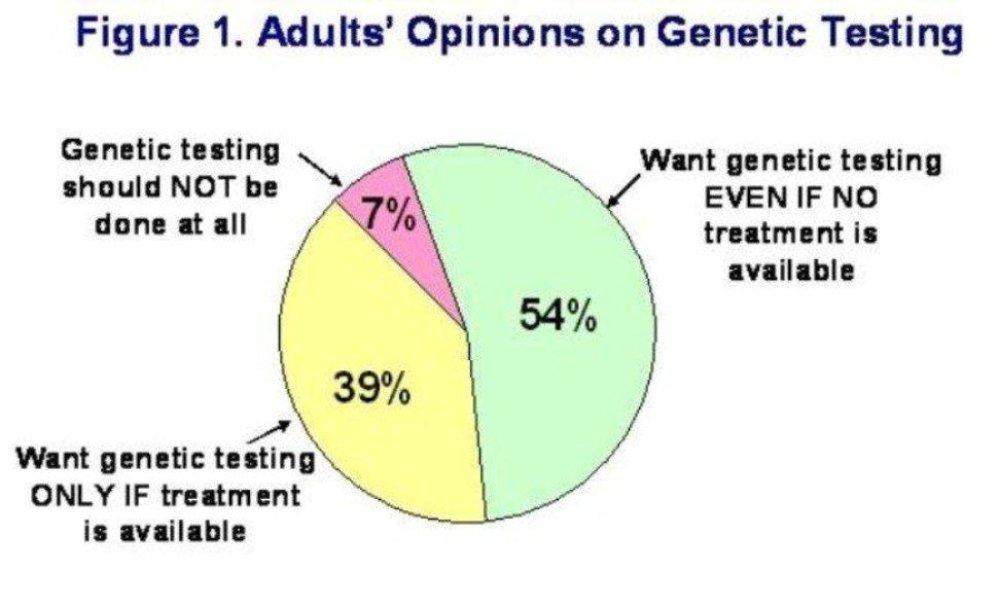   |